Healthy Aging for a Sustainable Workforce
Summary Statement
A report identifying important issues that revolve around construction’s aging workforce and its needs on the job and off.
2009
Conference Discussion Papers and Resources (Part 2)
Special challenges of aging
Ageing workers as a global condition – the European approach
The relationship between aging, job characteristics and health in
construction industry: some preliminary data from the Netherlands
Public policy options for an aging workforce
Health Care and Social Assistance (HCSA) Workers
Kathleen M. McPhaul, PhD, MPH, RN
Jane Lipscomb, PhD, RN, FAAN
University of Maryland
Work and Health Research Center
Baltimore, Maryland
Introduction
In 2004 the Institute of Medicine/National Academy of Science (NAS) Committee on Health and Safety Needs of Older Workers recommended improved data systems to track occupational exposures, injury and illnesses, and more research describing the health and safety needs of older workers. Furthermore, they pointed out that the field lacks clarity on the effectiveness of policies and programs which aim to improve the health of older workers (Wegman and McGee, 2004). These recommendations remain valid and compelling; but arguably the demographics of the healthcare and social assistance workforce together with the nature of human services and caregiving work require distinct research programs within the framework outlined in the 2004 NAS report. The purpose of this paper is to describe the healthcare and social assistance workforce, outline the well-documented safety hazards of this work, and conceptualize a research framework for older healthcare and social assistance workers.
Healthcare and Social Assistance Workforce
We examine the healthcare and social assistance workforce through the lens used by the National Occupational Research Agenda (NORA). NORA is a multi-disciplinary process organized by the U. S. National Institute for Occupational Safety and Health (NIOSH) to develop a national research agenda on occupational safety and health. The U. S. workforce is divided into sectors and stakeholders from labor, academia, government and industry. A group of stakeholders from the healthcare industry and worker representatives recently reviewed the state of the healthcare and social assistance (HCSA) workforce and research needs for health and safety (NORA, 2009).
In order to fully appreciate the significance of the healthcare and social assistance workforce, it is essential to understand the dimensions of the workforce and the nature of the work. The HCSA workforce employs approximately 17.4 million workers or 12% of the U. S. workforce (HRSA, 2008). This sector is adding jobs and projected to continue growing as the U. S. population ages. Within the sector, four subsectors were identified: (1) ambulatory care services, which employ 6.1 million workers, (2) hospitals, which employ 5.7 million, (3) nursing and residential care services, employing 2.5 million, and (4) social assistance, which includes 3.1 million. Notably, the social assistance sub-sector includes child day care service providers, individual and family services and food, housing, and emergency services (NAICS Code 62).
The work is characterized by direct contact with and care of needy, sick, and vulnerable populations, and involves caring for those who cannot fully care for themselves, whether due to age, illness, economic status, or developmental disability. Workers within the subsector of HSCA vary in level of education, training and socioeconomic status, and include medical professionals, social workers, nurses, drug counselors, day care providers, and home health aides, among others. Understanding the nature of this work is key to conceptualizing research questions on the impact of job exposures on older healthcare and social assistance workers. For example, working with institutionalized persons both in the long-term and acute care settings often involves physically demanding work, twelve hours shifts, night and weekend work, as well as an intense emotional component. Working in teams, which can offset some of the demands of the job, is common in the institutional setting, but not the community and home settings, which require mobility and offer less access to assistance, support, and security.
It is well documented that the U. S. health workforce is predominantly female and suffers from shortages amongst registered nurses, nurses aides, and other practitioners (Beecroft, 2008; Benjamin, 2008; Buerhaus, 2000 and 2008). Furthermore, the 2004 profile of the U. S. Health Workforce found that 18% of physicians are over 65 compared to 12.6 % of the general population. States such as California, Florida, and Arizona report that 20% of physicians are over age 65. Over 2.4 million registered nurses were employed in nursing in 2004; thirty-nine percent of Registered Nurses (RN) are 45 years or older, compared to the average of thirty-four percent for all jobs (Dohm, 2002). The average age of an RN is 47 years. These workforce demographics, combined with projections that the U. S. population has an increasing proportion of older individuals, especially those over 85, suggests that healthcare workers will be needed to work into older age to meet these demands.
As noted in other presentations, researchers vary in their definitions of “older.” Some examine workers over 45 years old, while others have used 50 and 55 to define “old.” In our view, the lack of age-specific injury and illness data by job title and other indicators of exposures for HCSA workers impedes the discussion of what age should be used to define “older HCSA workers.” In fact, until there is a general consensus on this issue, or more definitive evidence of an age-related effect within HCSA worker injuries, investigators will have to continue to use multiple cut off points and justify it according to the conceptual framework guiding their hypotheses.
Occupational Exposures and Hazards to HCSA Workers
Working conditions in today’s healthcare work environment contribute 16.3% of all non-fatal occupational injuries and 20.7% of all non-fatal illnesses reported to the Bureau of Labor Statistics (BLS, 2005 a, b, and c). Incidence rates for non-fatal occupational injuries are consistently higher in the healthcare and social assistance workforce than those for all private industries (e.g., 5.4 vs. 4.2 per 100,000 full-time workers in 2006). Similarly, incidence rates of non-fatal illnesses for healthcare workers are 40.0 vs. 24.6 per 100,000 full-time workers. While the hazards of the healthcare work environment are detailed in the 2009 State of the Sector report (NORA, 2009), a few will also be highlighted here. Already mentioned are the workforce shortages that contribute to the need for long working hours and overtime, and result in burnout. Other issues which impact the health and safety of the healthcare and social assistance workforce are a safety culture that prioritizes patient safety over staff safety, the frequency of emergencies which frequently circumvent safety processes (such as use of engineered lifting equipment), and the way that work is organized in some healthcare settings.
The hazards of healthcare work are well documented and fall into the broad categories of chemical, biological, biomechanical, physical, and psychosocial. Chemical hazards include toxic antibacterial cleaning chemicals and sterilants, as well as dangerous antineoplastic drugs. Biological hazards include possible exposures to HIV, Hepatitis B and C via bloodborne exposures, and airborne exposures, such as influenza, tuberculosis, and SARS. Contact exposures to antibiotic resistant organisms, such as MRSA and c-difficile, are also part of the job. By far the hazards that cause the most disability are the heavy lifting and awkward postures, resulting in musculoskeletal injuries associated with patient handling. Back and other musculoskeletal injuries account for the highest proportion of injuries in this sector, with the highest musculoskeletal injury rates occurring to nursing home aides and orderlies in long-term care. Radiation, noise, microwaves, and laser exposures are found in certain health care jobs, and finally, violence from patients toward workers is endemic in many healthcare and social service settings (NORA Draft Report, unpublished).
Impact of Age on the Health and Safety of Older HCSA Workers
Normal aging, combined with the classic work paradigm and occupational exposures of HCSA work, may adversely impact workers’ physical and mental health, quality of life, and the quality of patient or client care. The following suggested associations, with some exceptions, represent biological plausibility and deserve specific systematic investigation, but are not definitely described. For example, normal reductions in strength, coupled with a higher prevalence of joint pain in older adults, suggests that the physically demanding patient handling tasks in HCSA work will disproportionately impact older healthcare workers and increase pain and disability.
Similarly, older individuals are at higher risk of injuries from falls, further suggesting that the high incidence of slips, trips, and falls in healthcare work will impact older workers in the form of more severe injuries, lost work time, and disability. Normal decrements in balance, vision, and hearing may combine with the noise, interruptions, and poor lighting in many healthcare settings and result in stress, poor concentration, medical errors, and visual fatigue. Reductions in stamina may influence whether older workers can work twelve hour shifts, overnight shifts, overtime, or multiple days without time off. Finally, work and life balance may be more challenging for older healthcare workers who may be responsible for the care of older parents, disabled or ill spouses, as well as children and/or grandchildren (Silverstein, 2008).
The limited investigations of older healthcare workers suggest an age effect for increased injuries with night shift work and successive night shift work (Folkard, 2008). Furthermore, a 2006 survey of 308 RNs over fifty years old in two states showed that these RNs reported better overall physical and mental health than national norms, but also found that 36% reported work-related health problems and 23% reported work-related injuries over the past 5 years (Levtak, 2006). In a study of age and work schedule in 2273 RNs, the mean age was reported as 45 years, with 36.6% older than 50. Of the group fifty and over, 47.4% reported working more than eight hours per day, and 34.9% worked greater than forty hours per week, leading to concerns about safety for both the older nurse and the patients (Trinkoff, 2006).
The European NEXT study found that Work Ability scores were lower in older nurses in all ten participating European countries and that there is an association between low perceived work ability and intention to leave (Camerino, 2006). A Danish Nurses Study found that early retirement of nurses was predicted by poor health, lower income, having an unemployed spouse, and job condition (Friss, 2007).
The University of Maryland Work and Health Research Center examined data from studies of home care RNs in Maryland and personal care assistants in a home in Illinois. Older home care RNs (>50) are just as likely to rate their health good or better as home care RNs, who are younger than fifty. With respect to work hours, however, older home care RNs are more likely to work more than five days per week, more than forty hours per week, and more than five days per week in the field. Of note, older home care RNs also have more education, do less direct care, report receiving more respect from peers and supervisors and report less burnout and lifting (McPhaul and Lipscomb, unpublished).
Older personal care assistants (PCAs) who work in the home care setting are just as likely to rate their health as good or better as their counterparts who are less than fifty. There are no differences, however, between older and younger PCAs with respect to the number of hours and number of clients per week. Older PCAs are more likely to hold a second job. Older PCAs also reported getting more respect from clients’ families and clients themselves (McPhaul and Lipscomb, unpublished).
In terms of workplace violence, the exposure of workers to violent patients on the job, preliminary evidence suggests that age is protective for both home care RNs and PCAs. In addition, older PCAs report a greater level of comfort and confidence in working with difficult clients. These finding suggest that older RNs and PCAs possess valuable knowledge, demeanor, and skills in the interpersonal arena of caregiving, which must be explored further. Retention of older HCSA workers is desirable, but working conditions must also support a longer tenure in the workforce (McPhaul and Lipscomb, unpublished).
Stakeholders Input
A break out session moderated by the authors was attended by 30-40 stakeholders from industry, professional groups, occupational medicine and nursing, and healthcare unions. A set of questions and issues was used to organize the discussion, but the stakeholders were not limited to those issues. The following summarizes the themes from this discussion. Breakout Session Questions
Breakout Session Questions
Healthy Aging for Workers: Anticipating the Occupational Safety and Health Needs of an Increasingly Aging Workforce
HCSA Breakout Session
Moderated by Jane Lipscomb and Kate McPhaul
Defining “Aging” Workers
- * How do we best define 'aging' worker for the purpose of reducing work-related injury and illness?
- At what age do we start to see evidence of impairment?
- Is there an age at which older workers experience synergistic effects due to age and hazardous occupational exposures?
Organization of Work and Older Workers
- What aspects of organization of work are most important for aging HCSA worker?
- Can changes in organization of work help reduce work-related injury and illness among aging workers?
Occupational Health Practice
- Are there hazardous work exposures that are more dangerous for older workers ?
- Are there any important biomarkers or existing surveillance markers that should have lower “cut offs” and/or be monitored to prevent injuries in older workers?
- Are adult education approaches in occupational safety and health training adequate for older workers?
- What specific interventions can be applied now to preventing work-related injury and illness among aging workers?
- * What changes should companies consider in preventing work-related injury and illness among aging workers?
Policy Issues
- What disability issues are likely to be related to an aging workforce?
- * How can age discrimination be avoided with respect to preventing age-specific work-related injury and illness?
- Are aging workers adequately protected from work-related injury and illness by current occupational safety and health standards?
- * What opportunities are there for preventing work-related injury and illness among older workers as the Federal Government implements Economic Stimulus and Infra-Structure Re-building and other large scale programs?
Research Gaps/Questions
- * What are the most pressing questions that need to be researched to better protect the health and safety of an aging workforce?
- Are current work-related injury and illness and fatality surveillance systems adequate for monitoring an increasingly aging workforce?
Breakout Session Themes
Culture and Socialization of the HCSA Workforce
It is important to acknowledge that healthcare workers are predominantly female, and often view their work as a “calling” rather than a “job.” This phenomena may contribute to individuals within this workforce risking their own health on behalf of their clients. Others noted that it is important to understand the attitudes towards older workers within the institutions.
Some participants noted that there are important differences between older and younger HCSA workers. For example, “tech savvy” younger workers work side by side with older workers who may not value, appreciate or desire the technology available for communication, information retrieval, documentation and entertainment. Other differences include the fact that training needs and learning styles are different for older workers than younger workers.
Some noted that due to the economy and changing nature of the U. S. service sector that older workers are entering this field for the first time. Some note that currently there are high levels of job satisfaction among older workers. However is this also true in the HCSA sector, and if so will it persist?
From a personal health standpoint, older workers are more likely to have chronic diseases, which increases vulnerability to occupational exposures (e.g.lifting, pulmonary exposures) and also experience a decrease in immunity as they age. These health and medical differences between older and younger workers may be profound but may also be addressed in ways that keep this workforce as healthy as possible in their jobs.
Healthcare is a highly hazardous sub sector
Some in the audience articulated that the healthcare and social assistance sector is so hazardous that if the known hazards were addressed that the risks for all workers would be reduced. There was some sense that it is not aging per se, but the highly hazardous nature of the work that puts all workers at risk. There was also a sense that the physical demands of this work have increased and that work organization has intensified the physical and emotional demands of the work. For example, high staffing ratios, changing patient population (older, sicker, more overweight), working with insufficient staff, working alone forces workers to engage in dangerous and risky practices.
Ultimately, age does matter because at some point older workers can no longer perform the tasks required for the job.
Programs/ Interventions for Older HCSA Workers
It was suggested that the industry needs processes to incorporate health and safety into the work. Currently, adaptations and accommodations for older workers occurs informally, as in the case of surgeons and medical doctors who police older colleagues and either “cover” for them or move them into consultative roles with less direct care. Formal policies and programs that were suggested include:
- On-site Elder Care
- Flexible hours
- Variability in preferences of staff for shift length
- Group determination of schedule
- Accommodations for older workers responsible for elder care, just as accommodations are made for workers with young children
- Designing out hazards rather than training to avoid hazards
- Transportation for community-based workers
- Programs to reduce trips and falls
- Set expectations at practice could place aging workers at increased risk of unexpected hazards/events
- Severity of injury, increased recovery period/MD behavior on Return to Work (RTW) of older workers
Research and Data Issues
There is a dearth of quality data following this workforce for both exposures and outcomes related to working conditions or age. There was general agreement that there must be improvements in data quality for healthcare as a whole as well as improved indicators, which may be possible via increased use of electronic medical records.
Possible areas for future research include:
- Assessing the effectiveness of training and characterizing the learning styles of older workers.
- Do musculoskeletal injuries lead to migration from bedside? What are the subsequent consequences for patient/client care quality?
- Are low paid HCSA workers more likely to lose income with career ending injuries? Are they also less likely to have health insurance?
- What are best practices for Return To Work (RTW) from occupational and non-occupational injuries and illnesses for older HCSA workers?
- What are reasonable accommodations?
- RTW based on capacity to work, not disability Is there an increase in uninsured among the aging?
- Can we link patient data with worker data with improved electronic medical records? Will e-records introduce increased opportunities for surveillance and research?
- Characterize the contribution of older workers to patient care quality, patient safety, and as models and trainers of younger workers.
Final Impressions and Recommendations
- Recommendations from 2004 Institute of Medicine (IOM) report have not yet been implemented. The IOM framework provides a basis for specific sub-sector research recommendations which are urgently needed for high risk sub-sectors such as Health Care and Social Assistance (HCSA).
- The HCSA workforce is distinct in its high proportion of female workers, the inherently hazardous nature of the work, several decades of intensification of work, severe worker shortages, and the projections for rapid future growth.
- There is no universally agreed upon age that is currently considered the cut point defining the older worker, but 45, 50 and 55 have been used in recent investigations. Alternative paradigms for defining the older worker may be needed.
- Older HCSA workers appear to have similar work schedules as younger workers and some are working more than eight hours per day, more than 40 hours per week, as well as successive night and weekend shifts.
- There is some evidence that older RN’s are able to reduce the physical demands of their jobs; this must be characterized and understood in the context of exposure research and establishing the health and safety needs of older HCSA workers.
Given the enormous need for a skilled and experienced healthcare and social assistance workforce, research and policy should focus on those aspects of work that contribute to healthy aging while testing interventions to reduce the unhealthy impact of healthcare and social assistance work on this highly necessary and valuable workforce.
References
Beecroft, P. C., Dorey, F., & Wenten, M. (2008). Turnover intention in new graduate nurses: A multivariate analysis. Journal of Advanced Nursing, 62(1), 41-52. doi:10.1111/j.1365-2648.2007.04570.x
Benjamin, A. E., Matthias, R. E., Kietzman, K., & Furman, W. (2008). Retention of paid related caregivers: Who stays and who leaves home care careers? The Gerontologist, 48 Spec No 1, 104-113.
Braver, E. R., & Trempel, R. E. (2004). Are older drivers actually at higher risk of involvement in collisions resulting in deaths or non-fatal injuries among their passengers and other road users? Injury Prevention, 10(1), 27-32. doi:10.1136/ip.2003.002923
BLS [2005a]. Table SNR05, Incidence rate and number of nonfatal occupational injuries by industry, private industry, 2005. [www.bls.gov/iif/oshwc/osh/os/ostb1611.txt]. Date accessed: February 2008.
BLS [2005b]. Table SNR10, Numbers of nonfatal occupational illnesses by industry and category of illness, private industry, 2005. [www.bls.gov/iif/oshwc/osh/os/ostb1616.txt]. Dateaccessed: February 2008.
BLS [2005c]. Table SNR08, Incidence rates for nonfatal occupational illness by industry and category of illness, private industry, 2005. [www.bls.gov/iif/oshwc/osh/os/ostb1614.txt].Date accessed: February 2008
Buerhaus, P. I. (2008). Current and future state of the US nursing workforce. JAMA: The Journal of the American Medical Association, 300(20), 2422-2424. doi:10.1001/jama.2008.729
Buerhaus, P. I., Staiger, D. O., & Auerbach, D. I. (2000). Implications of an aging registered nurse workforce. JAMA: The Journal of the American Medical Association, 283(22), 2948-2954. doi:10.1001/jama.283.22.2948
Camerino, D., Conway, P. M., Sartori, S., Campanini, P., Estryn-Behar, M., van der Heijden, B. I., et al. (2008). Factors affecting work ability in day and shift-working nurses. Chronobiology International, 25(2), 425-442. doi:10.1080/07420520802118236
Camerino, D., Conway, P. M., Van der Heijden, B. I., Estryn-Behar, M., Consonni, D., Gould, D., et al. (2006). Low-perceived work ability, ageing and intention to leave nursing: A comparison among 10 european countries. Journal of Advanced Nursing, 56(5), 542-552. doi:10.1111/j.1365-2648.2006.04046.x
Camerino, D., Conway, P. M., van der Heijden, B. I., Estryn-Behar, M., Costa, G., & Hasselhorn, H. M. (2008). Age-dependent relationships between work ability, thinking of quitting the job, and actual leaving among italian nurses: A longitudinal study. International Journal of Nursing Studies, 45(11), 1645-1659. doi:10.1016/j.ijnurstu.2008.03.002
Chiu, M. C., Wang, M. J., Lu, C. W., Pan, S. M., Kumashiro, M., & Ilmarinen, J. (2007). Evaluating work ability and quality of life for clinical nurses in taiwan. Nursing Outlook, 55(6), 318-326. doi:10.1016/j.outlook.2007.07.002
Cohen, J. D. (2006). The aging nursing workforce: How to retain experienced nurses. Journal of Healthcare Management, 51(4), 233-245. Retrieved from http://onlinelibrary.wiley.com/doi/10.1111/j.1365-2648.2007.04530.x/abstract
Costa, G., & Di Milia, L. (2008). Aging and shift work: A complex problem to face. Chronobiology International: The Journal of Biological & Medical Rhythm Research, 25(2), 165-181. doi:10.1080/07420520802103410
Eriksen, W. (2006). Practice area and work demands in nurses' aides: A cross-sectional study. BMC Public Health, 6, 97. doi:10.1186/1471-2458-6-97
Estryn-Behar, M., van der Heijden, B., Camerino, D., Fry, C., Le Nezet, O., Conway, P. M., et al. (2008). Violence risks in nursing--results from the european 'NEXT' study. Occupational Medicine, 58(2), 107-114. doi:10.1093/occmed/kqm142
Folkard, S. (2008). Shift work, safety, and aging. Chronobiology International, 25(2), 183-198. doi:10.1080/07420520802106694
Friis, K., Ekholm, O., Hundrup, Y. A., Obel, E. B., & Gronbaek, M. (2007). Influence of health, lifestyle, working conditions, and sociodemography on early retirement among nurses: The danish nurse cohort study. Scandinavian Journal of Public Health, 35(1), 23-30. doi:10.1080/14034940600777278
Fuss, I., Nubling, M., Hasselhorn, H. M., Schwappach, D., & Rieger, M. A. (2008). Working conditions and work-family conflict in german hospital physicians: Psychosocial and organisational predictors and consequences. BMC Public Health, 8, 353. doi:10.1186/1471-2458-8-353
Gabrielle, S., Jackson, D., & Mannix, J. (2008). Older women nurses: Health, ageing concerns and self-care strategies. Journal of Advanced Nursing, 61(3), 316-325. Retrieved from http://onlinelibrary.wiley.com/doi/10.1111/j.1365-2648.2007.04530.x/abstract
Gabrielle, S., Jackson, D., & Mannix, J. (2008). Adjusting to personal and organisational change: Views and experiences of female nurses aged 40-60 years. Collegian (Royal College of Nursing, Australia), 15(3), 85-91.
HRSA [2008]. The registered nurse population: findings from the 2004 National Sample Survey of Registered Nurses. In: Health Resources and Services Administration.[http://bhpr.hrsa.gov/healthworkforce/rnsurvey2008.html]. Date accessed: February 2008.
Hwalek, M., Straub, V., & Kosniewski, K. (2008). Older workers: An opportunity to expand the long-term Care/Direct care labor force. The Gerontologist, 48(suppl_1), 90-103.
Ilmarinen, J. (2006). The ageing workforce--challenges for occupational health. Occupational Medicine (Oxford, England), 56(6), 362-364. doi:10.1093/occmed/kql046
Ilmarinen, J. (2006). Towards a longer and better working life: A challenge of work force ageing. La Medicina Del Lavoro, 97(2), 143-147.
Ilmarinen, J. (2009). Work ability-a comprehensive concept for occupational health research and prevention. Scandinavian Journal of Work, Environment & Health, 35(1), 1-5.
Janssen, P. P., Jonge, J. D., & Bakker, A. B. (1999). Specific determinants of intrinsic work motivation, burnout and turnover intentions: A study among nurses. Journal of Advanced Nursing, 29(6), 1360-1369.
Kuoppala, J., Lamminpaa, A., & Husman, P. (2008). Work health promotion, job well-being, and sickness absences--a systematic review and meta-analysis. Journal of Occupational and Environmental Medicine / American College of Occupational and Environmental Medicine, 50(11), 1216-1227. doi:10.1097/JOM.0b013e31818dbf92
Letvak, S. (2005). Health and safety of older nurses. Nursing Outlook, 53(2), 66-72. doi:DOI: 10.1016/j.outlook.2004.09.005
Rotenberg, L., Portela, L. F., Banks, B., Griep, R. H., Fischer, F. M., & Landsbergis, P. (2008). A gender approach to work ability and its relationship to professional and domestic work hours among nursing personnel. Applied Ergonomics, 39(5), 646-652. doi:10.1016/j.apergo.2008.02.013
Savinainen, M., Nygard, C. H., & Ilmarinen, J. (2004). A 16-year follow-up study of physical capacity in relation to perceived workload among ageing employees. Ergonomics, 47(10), 1087-1102. doi:10.1080/00140130410001686357
Shacklock, K., Brunetto, Y., & Nelson, S. (2009). The different variables that affect older males' and females' intentions to continue working. Asia Pacific Journal of Human Resources, 47(1), 79-101. Retrieved from http://apj.sagepub.com/content/47/1/79.abstract
Siddharthan, K., Hodgson, M., Rosenberg, D., Haiduven, D., & Nelson, A. (2006). Under-reporting of work-related musculoskeletal disorders in the veterans administration. International Journal of Health Care Quality Assurance Incorporating Leadership in Health Services, 19(6-7), 463-476.
Silverstein, M. (2007). Ergonomics and regulatory politics: The washington state case. American Journal of Industrial Medicine, 50(5), 391-401. doi:10.1002/ajim.20437
Silverstein, M. (2008). Meeting the challenges of an aging workforce. American Journal of Industrial Medicine, 51(4), 269-280. doi:10.1002/ajim.20569
Tuomi, K., Huuhtanen, P., Nykyri, E., & Ilmarinen, J. (2001). Promotion of work ability, the quality of work and retirement. Occupational Medicine (Oxford, England), 51(5), 318-324.
Ageing workers as a global condition – the European approach
Robert Anderson
European Foundation for the Improvement of Living and Working Conditions
Dublin, Ireland
Summary
This presentation begins with an overview of older workers’ employment in the European Union (EU) and considers why the extension of working life has become increasingly important in EU policies. Increasing attention is being given to the health of the ageing workforce and its maintenance through company initiatives. The following sections consider the working conditions and health risks of older workers in the EU, and examine the diversity of approaches to age management in European workplaces – specifically in the minority of companies which have implemented specific measures. The paper concludes with a series of key messages for policy and practice, acknowledging that there is an implicit research agenda throughout the discussion.
The European Foundation is a European Union agency working across all 27 EU Member States. Its work is primarily oriented to addressing social and employment policy issues, communicating messages to policy-makers in the European institutions and the social partners, employer and trade union organisations. The Foundation has been reporting on developments for the ageing workforce since the mid-1990s with a series of studies on good practice in companies and the working conditions of the ageing workforce. A series of reports and a database of good practice are available on the Foundation’s website (http://www.eurofound.europa.eu/research/0296.htm).
Older workers are first mentioned in EU documents in 1994 when they are identified as one of the key vulnerable groups in employment. Since the late 1990s, older workers have been the explicit focus of policy measures incorporated under the umbrella of the European Employment Strategy. The employment rate of older workers (defined in all EU policy documents as those aged 55-64) has increased fairly steadily over the last decade and is now approaching 45 percent. There are clear differences between the employment rates of male (54 percent) and female (36 percent) older workers; and while 40 percent of women aged 55-64 are working part-time, this applies to only 10 percent of men in this age group. However, the recent increases in employment rates of older workers are primarily a reflection of growing female labor force participation and correspondingly the older workforce is increasingly female. Incidentally, the employment rate of workers aged 65-69 in the EU is less than 10 percent compared with nearly 30 percent in the US.
Older worker employment rates are highest in the Nordic countries of Sweden and Denmark and are seen to be relatively high in the UK and Ireland as well. However, they are relatively low (below 40 percent) in some of the bigger Member States such as France and Italy, and are particularly low in some of the new Member States like Poland and Hungry. In part, the growing concern about employability of workers aged 55-64 reflects the fact that the age group 55-64 will grow over the next decade as a proportion of the working age population. But demographic change involves both an ageing workforce and an ageing population, and the impetus to increase employment rates among older workers is largely driven by concerns about the rapidly increasing numbers of people over the age of 65. However, there are significant differences between Member States in the projected changes in the working age and general population, with particular challenges in most of the new Member States.
The ageing workforce has moved higher on the European social policy agenda not only with regard to employment, but also because of concerns about the sustainability of pensions and healthcare and the maintenance of productivity and competitiveness. The primary focus of EU policies has moved from an orientation to tax and benefit structures towards practices of age management in workplaces and the labor market. An EU Directive to combat age discrimination is being implemented slowly in Member States and specific targets have been agreed upon for employment rates among older workers. In 2001, Ministers from the Member States agreed to increase the employment rate to 50 percent by 2010; in 2002, Ministers targeted an increase in the effective retirement age of five years by 2010. Neither of these targets is going to be achieved even if employment rates have risen markedly and the effective retirement age has increased by more than one year since 2002.
The EU debate is focused on increasing the proportion of workers staying in employment until the age of 65 – not about working beyond retirement age. Member State governments have implemented a range of new policy measures over the last decade, particularly addressed to reform of social protection systems. Changes in social security include: pension reforms, generally increasing statutory retirement ages to 65 or even 67; reduced access to early retirement; and reduced access to disability/incapacity schemes. Other measures include programs to encourage companies to promote health, as is particularly evident in Finland and in Germany, and collective agreements to adapt workloads for older workers like in the Netherlands. In many Member States governments have taken some initiative to change attitudes towards and among older workers through awareness campaigns.
The health of the workforce has been increasingly connected to the employment agenda, including a more recent focus upon the mental health of the workforce. Over the last decade there has been growing acknowledgement of poor health as an important reason for early exit and retirement or for exclusion from employment. This raises issues of prevention, disability management, and return to work.
In the EU in 2006 there were 57 million people aged 55-64 including 25 million employed, 1.5 million unemployed, and 30 million inactive. Among workers aged 55-64, a higher proportion were working part-time (especially women) than among younger workers but fewer were on fixed term contacts. A much higher proportion of older workers are self-employed and a greater number of older workers are employed in agriculture and fewer in industry. Altogether there are a somewhat larger number of older workers in skilled non-manual occupations and fewer in low-skilled non-manual than among the younger population aged 25-54. This reflects a tendency for higher skilled people to remain in employment longer than low skilled individuals. The exodus of workers (especially men) from heavy manual work is also reflected in the working conditions of older workers. Data from the Foundation’s Working Conditions Surveys demonstrate that workers aged 55-64 are less frequently exposed to physical risks to health than younger workers although the differences are relatively small. There is much interest of course in the psycho-social risks for health associated with work intensification and job insecurity but the evidence is that those older workers still in employment tend to report more job autonomy and somewhat less work intensity. This may be attributable to the “healthy worker effect” and the earlier exit of workers with high levels of work intensity – or perhaps the adaptation of work organization to ageing.
The Foundation’s research on good practice in age management looked for initiatives in public and private sector employers in both the mid 1990s and again in 2005-06. In many Member States good practice is relatively hard to find and it has been estimated that less than 10 percent of companies in Europe are ready, or even preparing themselves, for demographic change. Among the examples of good practice, it appears that initiatives for training and lifelong learning are the main focus of measures in Belgium, France, Greece, Italy and Spain, while attention to flexible working practices, work organization, and re-thinking of working time arrangement is more common in Austria, Germany and the Netherlands. Attention to health promotion and protection and to workplace design is most evident in the Nordic countries and, to a lesser extent, in Germany and the Netherlands. However, even in companies with positive approaches to age management, there are contradictions insofar as early exit policies may still also be in place and there are inconsistencies when measures are developed for some groups in the workforce but not for others. Relatively few organisations have comprehensive and integrated approaches to age management.
Good practice in health promotion and health protection has become more widespread over the last decade and tends to include regular check-ups as well as lifestyle health promotion and measures for more ergonomic workplace design. The good practice may be preventive or meant to compensate for physical/mental health problems. Nevertheless there is relatively little explicit mention of active disability management or rehabilitation and reintegration measures. In general, companies emphasize the goal of optimizing work processes and the organization of work to enable employees to perform well and to maintain their working capacity. Altogether the most common measures for age management in companies remain in the area of training and development, but there has been increasing attention to work organization and more flexible working time arrangements in particular. There is relatively little specific attention to low-skilled workers or to the increasing feminization of the workforce.
It appears that most companies have introduced age management as a result of market or business needs, primarily to avoid labor and skills shortages but also to retain experience and to maximize the return from investment in training. The changing circumstances that are influencing the business case are reflected in rethinking of priorities for age management over time and in evaluations of the value of investing in an ageing workforce. There have been very few systematic evaluations of the benefits of age management but interviews with both staff and managers in companies tend to emphasize improved health, increased job satisfaction, improved teamwork and better relations between workers and managers.
The further development of age management in organisations seems inevitable given the demographic imperatives. However, there remains considerable resistance to extending working life and a culture of early exit persists in many countries. There is a continuing need to change negative attitudes towards the employment and productivity of older workers among both staff and (younger) managers. The case for age management can be strengthened through more research to demonstrate its impact and monetary value; and this evidence is likely to become increasingly essential for the sustainability of initiatives in the harsher financial climate. Not only is there is a need to reinforce motivation and incentives, for management and workers to maintain working capacity of staff as they age, but to also support this orientation with effective professional services. A new role is emerging for both occupational and community health workers as part of a multidisciplinary service to maintain and promote health and to enable workers with health problems to return to work. The development of more effective practice will depend upon improved coordination between services, as well as between these services and the workplace. Support for workers with health problems demands continuity and consistency in active measures. Above all, improving opportunities for older workers hinges upon promoting more positive attitudes and combating discrimination.
In conclusion, the research on the ageing workforce in Europe underlines the diversity of situations in different sectors, countries, and groups in the workforce. The promotion of employment opportunities for older workers by public policy has contributed to the growing number of initiatives in companies. The evidence from good practice studies has shown that comprehensive approaches to strengthen, maintain and regain working capacity are possible and worthwhile; however, there is a need to extend awareness, commitment, and implementation. Policy-makers in Europe are learning that it is not enough to change exit and retirement policies – now is the time to invest in the health and employability of a changing workforce.
The relationship between aging, job characteristics and health in construction industry: some preliminary data from the Netherlands
Peter Hoonakker, Cor van Duivenbooden, Henk van der Molen
The U.S. construction workforce is aging: the average age of construction workers increased from 36 years in 1985 to 39 years in 2005 (Center for Construction Research and Training (CPWR), 2007). According to data from the Bureau of Labor Statistics (BLS, 2006), in 2001, there were nearly 1 million construction workers 55 years and older. A review of the literature on older workers in the construction industry by De Zwart et al. (1999) shows a focus on fatal and nonfatal work-related acute injuries and accidents, and inconsistent findings concerning the relationship of age with accidents and/or mortality. The few studies on Occupational Safety and Health (OSH) of older workers in construction industry show that older workers have more work-related health complaints, including work-related musculoskeletal disorders (WMSDs), lung disorders, skin disorders, and hearing loss as compared to white collar workers and younger construction workers; they are also more likely to receive medical treatment for these disorders (Arndt, et al., 1996; De Zwart, et al., 1999; Deacon, Smallwood, & Haupt, 2005; Holmström, Moritz, & Engholm, 1995; Hoonakker & van Duivenbooden, To be published; Nurminen, 1997). Older construction workers have been identified as a vulnerable group, but little is known about workplace and individual factors that increase their likelihood of experiencing OSH problems and the methods for supporting their productive and safe participation in the workforce.
De Zwart et al. (1999) reviewed the literature on job characteristics and aging of older workers in construction industry. Results showed that increasing age is associated with changes in physical and mental/cognitive work capacity, job satisfaction and work motivation, workload, and fatigue and recovery after work. The authors also compared job characteristics and health of younger and older workers in construction industry using questionnaire data, and found that older workers reported more health complaints than younger workers. For example, older construction workers more frequently reported to be tired, to have sleep problems, hearing loss, musculoskeletal complaints, and nervous complaints. Results regarding job characteristics were less consistent. With regard to working under time pressure, lack of job satisfaction, and job future uncertainty, older workers reported more complaints, however, older construction workers reported fewer complaints about physically demanding work (De Zwart, et al., 1999). Unfortunately, in this study, the relation between job characteristics and health problems was not examined. Hoonakker & van Duivenbooden (To be published) conducted a 10-year monitoring study of older construction workers (see next paragraph). Results are in line with De Zwart et al.: older workers have significantly more health complaints than younger workers, but not necessarily more complaints about job characteristics. However, in both studies, the relationship between aging, job characteristics and health was not examined.
Preliminary Studies
Figure 1: Construction Site Workers with Complaints about Working in Awkward Postures by Age Categories, 1993-2003, in percentages
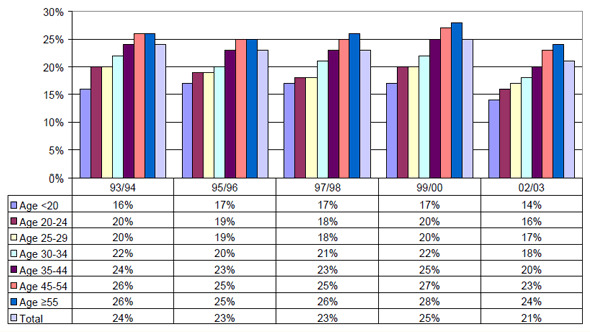
In an international collaboration with the Arbouw Foundation in the Netherlands, we used data from the Arbouw VISA database, a large database created by the Arbouw Foundation to examine job characteristics and health of construction workers. The VISA database contains data on job characteristics and OSH that are collected from more than 30,000 construction workers on a yearly basis; this data collection effort began in 1993 and is still on-going. The design of the VISA database makes it possible to monitor job characteristics and OSH in construction industry, and to compare different occupations, age groups, company size, etc. Thus, the surveillance process can be used to identify risk factors and risk groups, and to recommend interventions at the national and organizational levels. Furthermore, monitoring job characteristics and OSH over time facilitates the evaluation of these interventions (Hoonakker & van Duivenbooden, 2006b).
Using data from the VISA database in The Netherlands, Hoonakker and his colleagues (Hoonakker, 2000, 2001, 2005; Hoonakker & van Duivenbooden, 2006a) analyzed changes in job characteristics and health of construction workers from 1993-2003. Results show that many job characteristics have improved over the last 15 years. However, the improvement in job characteristics did not result in improved health of the construction workers: most health complaints increased in the last 15 years (Hoonakker & van Duivenbooden, 2006a). This may be a result of the rapidly aging workforce, possible long-term effects of prolonged exposure, or other factors. Recently, using VISA data from 1993-2003, we compared younger and older workers with regard to musculoskeletal health (Hoonakker & van Duivenbooden, to be published). Results show that working in awkward postures (standing for a long period of time, working in the same posture for a long period of time, and working in a stooped position) was reported more frequently by older workers (see Figure 1). Results also show that the age category 45-54 years old, and to a lesser extent, the age category 35-44, report nearly as many complaints as older workers (age 55 years and older).
Figure 2: Construction Site Workers with Health Complaints about the Upper Extremities by Age Categories,1993-2003, in percentages
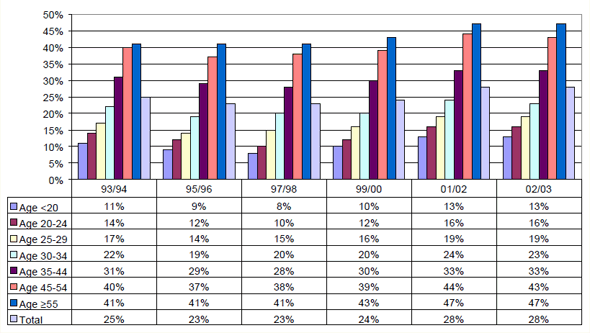
Results show that musculoskeletal disorders increase with age (see Figure 2). Complaints of the upper extremities have increased in the period 1993-2003. Older workers (55 years and older) report more complaints than workers in any other age category. All of these results are statistically significant. Preliminary analyses of the VISA database show that older construction workers have significantly more health complaints than younger workers. However, these studies used the repeated cross-sectional design of the VISA database. They do not help to determine whether the increase in complaints about job characteristics and musculoskeletal health is due to aging or to prolonged exposure to adverse job characteristics. We have also examined the longitudinal relationship between exposure to physical workload and environmental factors, and self-reported musculoskeletal disorders of the upper extremities among blue-collar construction workers (Hoonakker, van der Molen, & van Duivenbooden, 2007). Results show that, after controlling for age at baseline, exposure to a high physical workload, working in awkward postures and climatic factors are related to musculoskeletal disorders of the upper extremities as reported five years later. All of these results are statistically significant.
Figure 3: Construction Site Personnel with Health Complaints about Upper Extremities by Working in Awkward Postures,1993-1998, in percentages
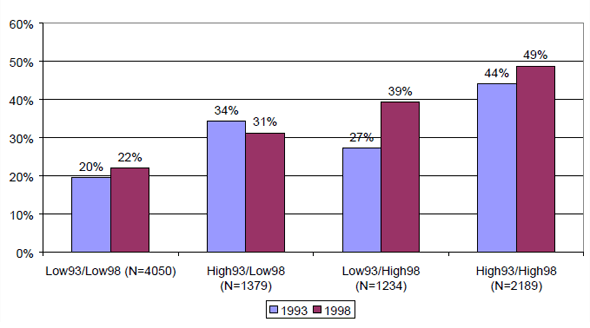
We have begun to examine the combined effects of age and exposure to physical workload on musculoskeletal disorders of the upper extremities. Preliminary results show that the increase in musculoskeletal disorders over a 5-year period is due to aging and exposure (see Figure 3). Results show the combined effect of age and exposure between 1993 and 1998 in a sample of nearly 9,000 blue collar construction workers. Construction workers with low exposure to working in awkward postures in both 1993 and 1998 reported a small increase in complaints of the upper extremities in the period 1993-1998 (from 20 percent to 22 percent). We can assume that the increase in complaints is due to aging. Interestingly, workers who reported high exposure to working in awkward postures in 1993 and low exposure in 1998 had a decrease in complaints of the upper extremities (from 34 percent to 31 percent). This suggests that exposure to working in awkward postures has a stronger effect than aging, and more importantly, once exposure decreases, workers reported fewer complaints of the upper extremities. The group of construction workers who reported low exposure to working in awkward postures in 1993 and high exposure in 1998 had the highest increase in complaints of the upper extremities between 1993 and 1998 (from 27 percent to 39 percent). This suggests a strong, combined effect of aging and exposure. Finally, the group of construction workers who reported high exposure to working in awkward postures, both in 1993 and 1998, had the highest percentage of complaints of the upper extremities of all groups (from 44 percent to 49 percent). The differences between the groups are statistically significant. This begins to demonstrate the effect of prolonged, high exposure to negative job characteristics such as working in awkward postures.
References
Adams, P. F., Hendershot, G. E., & Marano, M. A. (1999). Current estimates from the National Health Interview Survey, 1996. Hyattsville, Md.: U.S. Dept. of Health and Human Services, Centers for Disease Control and Prevention, National Center for Health Statistics.
Arndt, V., Rothenbacher, D., Brenner, H., Fraisse, E., Zschenderlein, B., Daniel, U., et al. (1996). Older workers in the construction industry: results of a routine health examination and a five year follow up. Occupational & Environmental Medicine, 53(10), 686-691.
Bureau for Labor Statistics(BLS) (2001). Current Population Survey.
Center for Construction Research and Training (CPWR) (2007). The Construction Chart Book (4 ed.). Silver Spring, MD: CPWR Publishing.
De Zwart, B. C., Frings-Dresen, M. H. W., & van Duivenbooden, J. C. (1999). Senior workers in the Dutch construction industry: A search for age-related work and health issues. Experimental Aging research, 25(4), 385-391.
Deacon, C., Smallwood, J., & Haupt, T. C. (2005). The health and well-being of older construction workers. International Congress Series, 1280, 172-177.
Holmström, E., Moritz, U., & Engholm, G. (1995). Musculoskeletal disorders in construction workers. Occupational Medicine: State of the Art Reviews, 10, 295-312.
Hoonakker, P. L. T. (2000). The Arbouw-Monitor: working conditions and health in construction industry 1989-1999. Amsterdam: Arbouw.
Hoonakker, P. L. T. (2001). Monitoring working conditions and health in construction industry 1989-2000 (De Arbouw-Monitor: Analyses op de PBGO-bestanden 1989/1990, 1993/1994, 1995/1996, 1997/1998, 1999/2000) (No. 02-07). Amsterdam: Arbouw.
Hoonakker, P. L. T. (2005). Arbouw Monitor 2005: Fiveteen years of monitoring working conditions and health in construction industry 1989-2003 (Arbouw-monitor 2005: analyses op de PAGO-bestanden 1989-2003. Monitoring van 15 jaar Arbeid en Gezondheid in de bedrijfstak bouwnijverheid (No. 05-78). Amsterdam: Arbouw.
Hoonakker, P. L. T., van der Molen, H. F., & van Duivenbooden, J. C. (2007). The relation between physical workload, environmental factors and musculoskeletal disorders of the upper extremities: A longitudinal study. Paper presented at the PREMUS Conference.
Hoonakker, P. L. T., & van Duivenbooden, J. C. (2006a, July 10-14). Monitoring working conditions and health in construction industry. Paper presented at the International Ergonomics Association, Maastricht, NL.
Hoonakker, P. L. T., & van Duivenbooden, J. C. (2006b, June 11-16). Monitoring working conditions and health of older workers in construction industry. Paper presented at the 28th International Conference on Occupational Health (ICOH), Milano, Italy.
Hoonakker, P. L. T., & van Duivenbooden, J. C. (To be published). Monitoring working conditions and health of older workers in Dutch construction industry. American Journal of Industrial Medicine.
Nurminen, M. (1997). Reanalysis of the occurrence of back pain among construction workers: Modeling for the interdependent effects of heavy physical work, earlier back accidents, and aging. Occupational & Environmental Medicine, 54(11), 807-811.
Public policy options for an aging workforce
Michael Silverstein, MD, MPH
University of Washington
Seattle, Washington
The aging of the baby boom generation has begun to produce profound changes in our workplaces. The impact of this generational shift will escalate as the leading edge of this huge cohort enters its sixties, still relatively healthy and increasingly eager (or resigned to the need) to continue productive work.
Yet the policy framework for addressing age at work, fashioned largely by the Employee Retirement Income Security Act (ERISA) of 1964 and the Age Discrimination in Employment Act (ADEA) of 1967 has been essentially static for years. It has been a framework of laws, regulations, and collective bargaining agreements intended to support and encourage a societal expectation since World War II that the generational torch will be passed at a relatively young age. This disparity between twentieth century vision and twenty first century needs has become progressively more evident.
I recently read the proceedings of a symposium that captured quite well this mismatch and the challenge it presents. “The presidential campaign...focused attention on the socioeconomic system of the United States. Little attention, however, was directed to an important issue: the aging of the American work force. Yet this phenomenon will have a significant impact on the national economy and is already being felt today... In light of the changing demographic picture and increased longevity, much more serious consideration should be given to any number of policy initiatives ... both to preserve employment opportunities ... and to facilitate a more satisfactory transition to retirement ....” 3, 4
While this could easily have been written to keynote this conference, it is actually from a 1988 symposium sponsored by the Big Three auto companies, the United Automobile Workers and the U.S. Department of Labor. While the participants did a nice job of articulating the pressing policy needs, it is clear that these needs were not fully appreciated. More than 20 years later they have still been largely unaddressed.
To drive home the point that we often do better at describing problems than responding to them, here is what the Bureau of National Affairs said in 1987. “The U.S. seems unprepared to deal with the complex challenges presented by the unprecedented influx of older Americans into the workforce in the coming decades. While some corporations and governments have initiated “activist” approaches toward older workers, in general, no coherent, coordinated public or private policies have been developed in response to this projected domination of the workforce by older workers.” 5
Twenty years later, in 2006, an AARP survey of business executives found the situation essentially unchanged. 83 percent of 1000 executives agreed that workers approaching traditional retirement age will play a greater role in the U.S. workforce over the next decade than previously. But, “despite an overall awareness of the potential implications of the aging workforce, few companies have taken action to prepare.” 6
The two major developments recognized in the 1980s have become more apparent every year.
First is the impending labor and skills shortage, illustrated by the plain population arithmetic that projects between 2006 and 2016 an 83 percent increase in the 65-74 year old group and a 7 percent drop among the 16-24 year olds. In Washington State, for example, between 2005 and 2025 there will be an increase of more than 250,000 65-69 year olds and a decrease of nearly 50,000 45-49 year olds.
Second, alongside this shift in the labor market, is the increasing fragility of our social security and private pension systems as the ratio of young workers to older retirees drops and the longevity of the retirees continues to increase.
There are four ways we might try to address these pressures.
- The first is to increase immigration of young workers, both skilled and unskilled.
- Second is to outsource work to international labor markets.
- Third is to increase reliance on automation and advanced technology to enhance productivity.
- Fourth is to delay retirement and retention of older workers.
We will certainly see proposals in the first three areas - such as guest worker programs or subsidies for automated technologies. While this will generate policy questions worth careful consideration, it is beyond the scope of this paper - except to note that while immigration and outsourcing may address some business concerns, they will not meet the needs of workers who are confronting the physical and cognitive changes of aging and must choose between continued work or retirement in the face of escalating health care costs and diminished pension security.
The fourth scenario, delayed retirement of older workers, is already well underway. For businesses this is a matter of competitiveness, skill retention, and pension costs. For individual workers it is partly the rational response to economic need and partly a choice about adapting work-life balance to increased longevity.
It is worth noting that while the pressures on workers to consider staying employed longer have been growing for some time they have sharply increased in just the past year. For example since the early 1990’s defined benefit pension plans have become less common and defined contribution plans more common. While this trend would have made some workers consider delaying retirement under any circumstances, the current economic crisis has made the riskiness of market-dependent retirement income an immediately frightening reality.
While it appears inevitable that more workers will opt to keep working longer, and while some public and private incentives to do this have already emerged - for example the phased increase in the age for full social security benefits and the decrease in the post retirement earnings penalty – it remains the case (as noted by the US Senate Special Committee on Aging) that “barriers in pension law, shortcomings in job training programs, and family caregiving commitments make it difficult for older workers to keep working.” 7
In thinking about how to address these barriers and shortcomings it is going to be important to keep two questions in mind:
First, can we ensure that policies intended to keep people at work longer will not have adverse consequences? (e.g., we could make longer careers more attractive by fully eliminating annuity offsets for employment after retirement) and Second, can we make early retirement less attractive? (e.g. by eliminating retiree health insurance benefits).
While both approaches discussed above might be equally effective in retaining older workers, the consequences for the workers themselves would be quite different. For instance, many defined benefit pension plans encourage relatively early retirement by capping benefits even if employees continue to work. An alternative to accomplish the same thing with less adverse consequence to the employee might be to change the accrual structure of a defined benefit plan so that there would be a net gain to staying another year or two, such as was done in the reform of the Finnish pension laws in 2005. 8
Equity is a related concern. Employers may wish to retain older workers by offering them phased retirement options, but only for those who are especially “valuable” because of their skills, knowledge or work habits – these most valuable employees tending to be highly compensated managers. Such selective benefits might seem to discriminate against other workers perceived by the employer to be less valuable but who are in equal or greater need of continued employment to meet their basic needs. However, current U.S. law may allow such programs. Formal retirement plans under the ERISA law are prohibited from favoring highly compensated employees. Knowing this, many employers have chosen to offer special phased retirement opportunities on an informal and ad hoc basis to selected individuals outside the legal framework of ERISA. To date the ADEA has not been an effective tool in addressing the discriminatory nature of these policies.
Finally, how do we ensure that workers extending employment past traditional retirement age can do so in a working environment that allows them to perform safely and productively to the end of their careers?
There is a body of evidence, particularly work done by Ilmarinen and colleagues at the Finnish Institute of Occupational Health, suggesting that attention to four general dimensions of worklife can maintain work ability as people become older on the job and can prolong the period during which they can continue to work safely and productively. 9
The first policy dimension is the work environment, the way that the physical, cognitive and organizational demands of work match worker capabilities. Injuries, disability and poor job performance are more likely when the physical requirements of work exceed individual capabilities, a mismatch potentially more frequent among older workers. Workplace ergonomics, human factors engineering and the principles of “universal design” can help young workers to reach older ages without injury and older workers to continue work without further harm.
Cognitive function also varies with age, particularly in the areas of complex problem solving and multitasking. Training programs, instructional materials, supervisory styles, workplace displays and signals all need to take these differences into account.
The way work and workplace relationships are organized also affects the ability of employees to perform safely and productively. Important factors include work schedules, supervisory relationships, decision control, and avenues for conflict resolution. For example, lower injury rates are associated with job autonomy, positive labor relations, low stress, low grievance rates and long-term commitments to the workforce. 10
Policy attention to the job environment should include the following:
- Incentives and/or requirements for workplace ergonomics and human factors programs.
- This could come about through:
- legislation (e.g. the safe patient handling requirements in Washington State);
- increased OSHA enforcement of the “general duty” of employers to keep workplaces free of recognized hazards;
- or rulemaking to require age friendly workplaces. The rulemaking option is particularly challenging because of the invocation of the Congressional Review Act to invalidate OSHA’s ergonomics rule and prohibit further regulations that are “substantially similar.”
- Incentives and/or requirements for measures that make work organization more age friendly. Examples include limitations on mandatory overtime or worker participation on safety and health committees that are free from management domination.
The second policy dimension focuses on individual needs for disease prevention and health promotion. Five chronic diseases more common with aging (heart disease, cancer, stroke, chronic obstructive lung disease, and diabetes) cause almost 70 percent of all deaths. Expenditures for employees just at risk for these diseases – measured by blood pressure, body weight, and cholesterol – averages over 50 percent more than for those at low risk. Other chronic non-fatal problems of aging, such as arthritis or hearing loss, add enormous medical costs and indirect impacts of absenteeism, low productivity, employee turnover and replacement.
While workplace wellness programs have proliferated, there is a strong evidence base for only a limited set of clinical service interventions. Among those recommended by the U.S. Preventive Services Task Force are influenza immunization, colorectal cancer screening, mammography, cholesterol and blood pressure screening, which can prevent or delay disability from chronic conditions by as much as 10 years, especially when supplemented by not smoking, eating a healthy diet and moderate physical fitness.
The design of health insurance benefits can inadvertently discourage the use of these preventive services of proven value. There is evidence that small deductibles or co-pays will significantly reduce the utilization of colon cancer screening services. Such cost control measures are short sighted and should be eliminated.
Insofar as health insurance premiums increase with age, employers who choose to provide health insurance benefits may be disinclined to hire or retain older workers. If a new national health program were to mandate employer coverage, it would be important to avoid discrimination by making it clear such practices would be subject to sanctions under the Age Discrimination in Employment Act.
Current Medicare rules discourage the retention of workers who want to continue full or part time work after age 65. Because Medicare is the secondary health care payer employers who provide health care coverage have an incentive to not hire or retain these workers or to discontinue the company health insurance program. We need a careful policy review of the pros and cons of making Medicare the primary payer or allowing private benefits to wrap around Medicare by reducing some of the private benefits as long as the total package is not diminished.
The third policy dimension addresses flexible work arrangements with options for the way that work-life balance is achieved, that take into account employee needs that change with age, particularly as they confront the realities of increased longevity, long term health care needs, decreased pension fund stability, and multi-generational family demands. The University of Michigan Health and Retirement Study has consistently shown that three out of four older workers would prefer to reduce hours gradually and stay longer rather than retire abruptly. 11 Large numbers are also interested in alternative job designs like flexible hours, job sharing, seasonal work, or telecommuting that reduce job stress and allow them to balance obligations and interests within and outside work. Many would like to continue full or part time work after they begin to draw social security and private pension checks.
Notwithstanding these strong worker interests in flexible arrangements, often shared by employers who need the continued contributions of older employees, they have not flourished. As mentioned earlier, even among the largest employers formal phased retirement programs are hard to find.
Policy needs include:
- the ability to begin receiving pension payments before age 62 while still working part time,
- the ability to reduce working hours in late career without a reduction in eventual pension benefits,
- and the continued eligibility for health care and other benefits if working hours are reduced in late career.
Many workers would like to be able to transition to part time work in their late fifties but are unable to do so unless they can begin to draw money out of their pension accounts to supplement their part time wages. Prior to 2006 the federal tax code and pension laws prohibited such “in service distributions” from defined benefit pension plans unless the employee had reached full retirement age (usually 65) or had fully terminated employment and took work elsewhere.
The Pension Protection Act of 2006 loosened these rules slightly, allowing distributions at age 62 (but not earlier) without terminating employment, even if this is before normal retirement age. Since 2004 a proposed change to IRS rules would take this one step further by allowing employees over the age of 59 ½ to reduce their hours by at least 20 percent while beginning to receive a percentage of their retirement benefits.
There are other disincentives to delayed or phased retirement that require policy solutions. For example, while it is easier to take money out of a defined contribution than a defined benefit pension plan while still working, this can only be done with a significant tax penalty if done before full termination of employment or age 59 ½. Also, many pension plans are specifically designed to discourage longer careers, for example by accruals that turn negative when workers are in their late fifties – i.e. the increased pension earned by working an extra year does not compensate for the fact that the person will get one less year of benefits. Many pension plans discourage workers who want to extend their careers with a few years of part time work before full retirement by calculating pension benefits based on the average earnings during the last 3-5 years of employment. If these plans modified the calculation to the highest 3-5 years of consecutive employment workers would not be penalized for reduced hours at the end of their careers.
A note of caution is warranted here. While early “in service” pension distributions may make flexible, phased retirement possible and attractive, they can have significantly adverse long term consequences for workers if they trade the early benefit for a reduction in the amount of final pension benefits when the worker fully retires. Very careful attention to the details of pension design will be needed to prevent “sleight of hand” plans that give with one hand and take with the other.
The fourth policy dimension is the social context of work. Many daily living tasks become more challenging with aging and can interfere with successful job performance. For example, older workers who no longer can drive to work easily have greater needs for public transportation, car pools, or telecommuting. Also, evolving family needs may become a significant distraction at work. An employee may not be able to function adequately at work without knowing that assisted living or home health care options are available for an older parent or spouse. While some measures to address these needs may be within the reach of individual employers (e.g. work-based car pools or elder care benefits), some must be addressed as broader social services such as improved access to health care, public transportation and laws to protect against discrimination
Plans for revitalizing our economy and rebuilding our infrastructure need to take into account aging at work, for example through development of regional and local public transportation systems rather than highway construction and a health care system that provides sufficient care for the elderly, allowing older workers with very old parents to continue working rather than caretaking.
With these four general strategies as context we can turn to more specific policy considerations. There is a need for new legislation. Two bills introduced in 2007 should be reintroduced and acted upon by the new Congress.
The Older Worker Opportunity Act of 2007 (S709) would:
- Amend the Employee Retirement Income Security Act of 1974 (ERISA) to extend COBRA continuation coverage for certain older workers.
- Amend the Workforce Investment Act of 1998 to take age into account (as one “hard to serve” population) in providing statewide and local employment and training services
- Direct the Secretary of labor to identify best practices for hiring and retaining older workers
The Health Care and Training for Older Workers Act (S708) would provide a tax credit of 25 percent of (first $6000 of) wages for employing older workers (62+) in formal flexible work programs that provide a full- or part- time flexible schedule and full pension and health care benefits. No discrimination in favor of highly compensated employees would be permitted.
Also, existing laws may need more effective enforcement. The Age Discrimination in Employment Act has been in place since 1967 (with subsequent amendments that lowered the age of coverage from 65 down to 40) and is administered by the Equal Employment Opportunity Commission (EEOC). The Act eliminated a number of age-based practices, including mandatory retirement age, denial of participation in benefit programs and retirement plans based on age. While insurance benefits must be provided on an equal benefit or equal cost standard, it is lawful to provide some reduced benefits to older workers if this equalizes the costs for benefits to younger workers.
As the numbers and percentages of older workers continue to grow, special vigilance needs to be directed to the way this Act is interpreted and enforced. Although the Act protects against discrimination in hiring and work practices, complaints and litigation have concentrated on termination from work (discharges and layoffs). This is likely to change as more older workers remain on the job and experience concerns about flexible work arrangements, retirement options, physical and cognitive stresses, and chronic illnesses. Discrimination in hiring and conditions of employment may be harder to prove than unfair termination because of the difficulty in identifying an affected class of employees. Statutory changes may be required to anticipate and address this. 12
There may also be new scenarios for discriminatory discharge cases. As pension funds shift from defined benefit to defined contribution designs older workers will be inclined to stay on the job longer. If employers intended this incentive for senior workers there will be no problem, but some employers who change pension plans just for an economic advantage may be unhappy when older workers stay on the job. The EEOC will need to be watchful for increased discriminatory discharges under these circumstances.
Some concluding remarks are needed to place these issues in the context of the larger changes that are approaching as the new administration and Congress wrestle with proposals for economic recovery. There should be little doubt that we will see more incentives, both public policy and private, to slow down the retirement of baby boomers, even as businesses contract in the crisis. It is in just such circumstances that adverse, unintended consequences become most possible. It will take the utmost care to ensure that workers are treated fairly and that we do not sacrifice their dignity and health in our zeal for emergency fixes to our financial systems and business models.
We need special watchfulness in three areas. First, can we encourage longer careers by rewarding delayed retirement instead of penalizing early or traditional retirement? Second, can we anticipate and prevent opportunities for age discrimination? Third, can we ensure that those workers who choose to work longer are able to do so in age friendly environments that enhance their work ability, safety, and health?
Designing the age friendly workplace of the future is a much more active process than formulating policy objectives. It means developing and implementing specific action plans with measurable performance objectives in each of the four areas I described earlier: the work environment, attention to individual health promotion and disease prevention, flexible work arrangements, and the social context of work. There is a need for some practical tools to help organizations put such action plans in place. One such tool that I have been working on for some time together with colleagues at the UW and the WA Department of Labor and Industries is a two day hands on workshop for the design of an age friendly workplace. You may have seen the poster session on this workshop and have talked about this with my colleague Ken Scott.
In closing it is worth a reminder that the concerns I have raised have been expressed repeatedly for more than twenty years. The “to do” list from the same 1987 Detroit conference that provided the opening to this talk is a fitting way to close it.
“First, there should be provisions for the continuous education and training of workers... Second, jobs and work environments can be redesigned according to ergonomic criteria which take into account the physical capabilities and limitations of individual workers. Third, older workers should be given opportunities to scale down their level of work involvement through job sharing, part time jobs and other kinds of reduced work schedules... Fourth, there should be provisions for pension portability...” 13
Now, in 2009, it would be a fine time to actually do some of these things.
One final reminder is that this is not about older workers. It is about the aging workforce. It’s never too late for new ways to prevent injuries and illnesses from happening or getting worse, but it is always better to start young.
_________________________________________________________
3 Bluestone I, Montgomery R, Owen J eds. The Aging of the American Work Force: Problems, Programs, Policies. Wayne State University Press, Detroit, 1990.
4 Stepp J. Older workers, new problems, new opportunities. In Bluestone I et al. eds. The Aging of the American Work Force: Problems, Programs, Policies. Wayne State University Press. Detroit, 1990.
5 Bureau of National Affairs, the Daily Labor Report. 7/9/87.
6 Business executives’ attitudes toward the aging workforce: Aware but not prepared? Survey conducted by Business Week Research Services for AARP, October 2006
7 http://aging.senate.gov/issues/olderworkers/index.cfm
8 Forma P, Tuominen E, Vaananen-Tomppo I. Finnish Pension Reform and Intentions of Older Workers to Continue at Work. Finnish Centre for Pensions Working Papers 2006:2.
9 Since 1981, a quantitative Work Ability Index (WAI), derived from a standardized, self-administered employee questionnaire, has been used in this research. The WAI at baseline has been found to be associated with disability pensions and mortality at 4 and 11 years of follow-up. WAI scores are also associated with disability and sickness absence costs as well as self-reported quality and productivity. While there is an overall decrease of WAI with age, there are several potentially modifiable variables that have been shown to enhance or inhibit this general trend. Included among the variables associated with preservation or enhancement of WAI are a) adjustments in physical work environment (physical workload, repetitive motion, and regulation of one’s own work and breaks); (b) adjustments in the psychosocial work environment (flexible work schedules); (c) health and lifestyle promotion (physical exercise, risk factor reduction,; and (d) worker skills and competency building. This evidence regarding work ability, while substantial, is somewhat indirect and little has been done in the way of rigorous study to demonstrate the effectiveness of interventions based on this work. A more full discussion about this evidence base is found in Silverstein, M, “Meeting the Challenges of an Aging Workforce,” Am J Ind Med. Published Online: Feb 12 2008. DOI: 10.1002/ajim.20569.
10 Shannon H, Mayr J, Haines T. 1997. Overview of the relationship between organizational and workplace factors and injury rates. Saf Sci 26(3):291–317. Landsbergis PA. 2003. The changing organization of work and the safety and health of working people: A commentary. J Occup Environ Med 45(1):61–72.
11 Health and Retirement Study Participant Update, Winter 2008. University of Michigan Institute for Social Research.
12 Neumark D. Reassessing the Age Discrimination in Employment Act. AARP Public Policy Institute #2008-09 June 2008
13 Stepp J. Older workers, new problems, new opportunities. In Bluestone I et al. eds. The Aging of the American Work Force: Problems, Programs, Policies. Wayne State University Press. Detroit, 1990.


